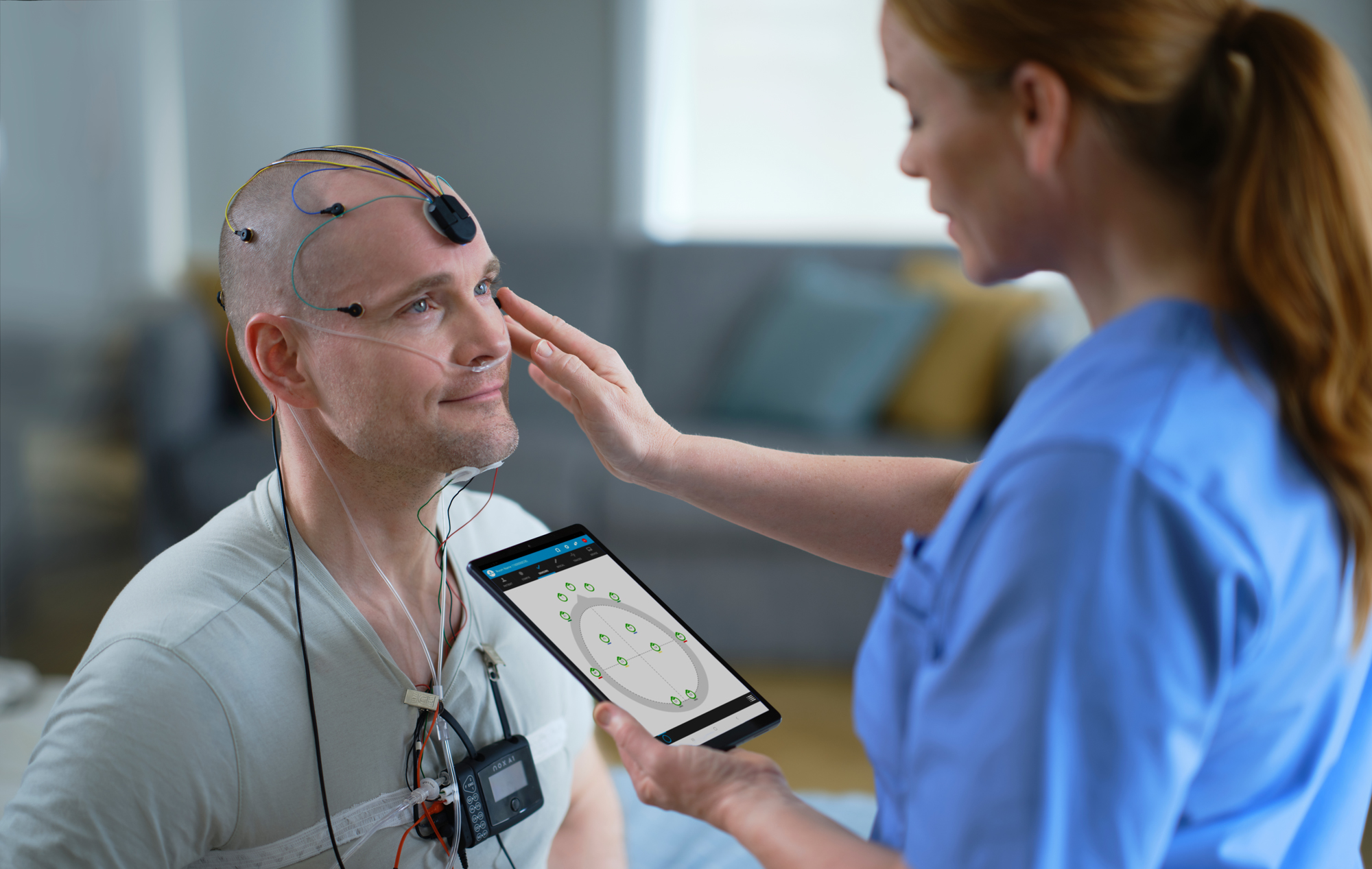
Clinical experts from Nox Medical share their insights on how to maximize patient comfort in the sleep lab to improve the accuracy of diagnostic testing.
No matter the location of where a patient may lay their head, the newness of a fresh sleeping environment seems to diminish restful sleep for many people. In fact, it is widely well-known and accepted that sleeping in a new environment for the first time will yield restless sleep. The phenomenon of poor sleep during a patient’s first night in a sleep lab during polysomnography (PSG) has even been dubbed the “first night effect.” Recordings during the first night are characterized by decreased total sleep time, lower sleep efficiencies, reduction in REM sleep, and longer REM latencies on the first night of testing.1
While the “first night effect” is still somewhat of a mystery, research reported in the journal Current Biology, helps explain why people tend to feel unrested after sleeping in a new place. The paper suggests that people who sleep in a new place frequently put half their brain to sleep while the other half remains on guard. Slow wave activity was greater in certain areas of the right hemisphere than in the corresponding areas of the left hemisphere, the study found.2
No matter the reason for the first night effect, sleep technologists throughout the globe have devised plenty of creative and easy ways to minimize the impact of the first night and ensure that patients get the most out of the diagnostic sleep testing, so they can get the most accurate diagnoses, the first time.
- Communicate openly with your patients
Give your patient the gift of open communication, says sleep technologist Jay Hemnani, RPSGT, who is the former sleep lab manager at FusionSleep in Georgia.
Patients often appreciate having some understanding of the reasons why they are going through the sleep testing process.
“First and foremost, it will come down to the mannerisms and the attitude of the technologist because I have seen it become very easy for the tech to normalize people coming in and having sleep studies, but very often for a patient it is the first time that have had anything like a sleep study done, so it is an unfamiliar experience for them,” says Hemnani.
“It is important for technologists to spend the time with patients to explain what they are doing, why they are doing it, what to expect throughout the night usually leads to easing some of that anxiety on the patient’s side,” he says.
- Bring the comfort of home to the sleep lab
If it is feasible, sleep lab managers may allow patients to bring a comforting support person to the sleep lab to sit by their bedside while they drift off to sleep. Some sleep labs have kitchenettes for when a patient might need a snack or a sip of water. Others might have pillow menus for patients to pick the pillow that most aligns with their pillow at home.
“A sleep lab is almost a cross between medical treatment and service industry in a way. If they are not comfortable, you are not going to get a good quality result,” says sleep technologist Byron Jamerson, RPSGT, a product specialist at Nox Medical.
“Anything you can do to make that patient more comfortable,” he says. “They are not at home; they are in a strange bed. Everyone is familiar with the first night effect. You just don’t sleep as well as you do at home.”
- Offer the patient a sense of control
Consider giving the patient some say in the temperature of the room. A cooler room is generally better for sleeping, but personal preference does play a part. Many sleep labs offer other ways that patients can control their environments, including offering adjustable mattresses with varying degrees of firmness.
“It’s all about getting your patient to sleep as normally as possible to get an accurate diagnosis,” says Jamerson.
- Minimize the bulk of the sleep study wires
Not all in-lab sleep diagnostic PSG studies require a bulky bundle of wires. New technological advances have led to much sleeker and light weight options, including the head cable that comes with the Nox A1s. “With the Nox head cable you don’t have a long, heavy, ‘ponytail of wires,’” says Hemnani, who is now a product training specialist at Nox Medical.
- Maximize the patient’s autonomy
“Given that it is an untethered experience with the Nox A1s, I do find that patients find the overall experience to be a little more comfortable. Patients are able to get up, move around, go to the restroom, without feeling like they are tethered to the nightstand or tethered to the equipment, and restricted” says Hemnani. When using other diagnostic sleep systems, oftentimes, the patient would wake up and just lay in bed for up to 15 minutes before calling out to the tech to go to use the restroom.
“It is a different kind of experience because you are used to being able to just get up and go,” he says. With the Nox A1s PSG, patients retain their independence and freedom to move.
References:
- Herbst E, Metzler TJ, Lenoci M, McCaslin SE, Inslicht S, Marmar CR, Neylan TC. Adaptation effects to sleep studies in participants with and without chronic posttraumatic stress disorder. Psychophysiology. 2010 Nov;47(6):1127-33. doi: 10.1111/j.1469-8986.2010.01030.x. PMID: 20456661; PMCID: PMC2925054.
- Tamaki M, Bang JW, Watanabe T, Sasaki Y. Night Watch in One Brain Hemisphere during Sleep Associated with the First-Night Effect in Humans. Curr Biol. 2016;26(9):1190-1194. doi:10.1016/j.cub.2016.02.063
Topic: Industry News