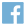The average time that a patient can expect to wait to get tested in a sleep laboratory in the United States is quite variable ranging from a few weeks to, in extreme cases, more than a year. According to estimates published in the American Journal of Respiratory and Critical Care Medicine, wait times for obstructive sleep apnea (OSA) diagnosis and treatment average between two to ten months. The number of untreated patients is only expected to grow as the number of board-certified sleep specialists continues to dwindle.
By using home sleep tests (HST) physicians can augment their services and see some of their patients’ test results faster, which can streamline diagnoses and lead to swift treatment plans, ultimately resulting in better patient outcomes. While polysomnygraphy (PSG) remains the gold standard, and is necessary for monitoring certain patient populations, home sleep tests offer a solution to help identify the many people who live with undiagnosed obstructive sleep apnea who might not find an in-lab sleep test comfortable or convenient.
“HST can clearly be more cost-effective for certain patient groups, given that the sleep study gives an accurate diagnosis. It is very important to gather as much input as possible for this to happen, along with very good data processing on the other end when analyzing the data,”
says Snorri Helgason, product manager at Nox Medical.
The Benefit of Home Sleep Testing
When determining whether to administer an in-lab sleep test versus an at-home sleep study, practitioners need to evaluate how much data is being jeopardized moving the sleep study to the patient’s home. HST vendors are slowly waking up to the fact that it’s not necessary to sacrifice as much data input as has been done in the past, says Helgason.
“HST should be more cost-effective than in-lab sleep studies. But this relies on some parameters. First, the cost of misdiagnosing a patient with HST, requiring an in-lab PSG follow up skews this picture. This then in return requires the HST to be more accurate. Second point is the duration of waiting for a treatment, how much will that affect the patient in terms of healthcare utilization, untreated OSA, etc.”
It’s important to diagnose these patients quickly because untreated OSA can lead to more severe comorbidities, including an increased risk of hypertension and atrial fibrillation, which can lead to higher healthcare costs and even mortality.
Additionally, since most at-home sleep tests are used just for one night, they are less expensive than a sleep study in a lab, Susheel Patil, MD, PhD, clinical director of the Johns Hopkins Sleep Medicine Program, says in a statement. “It’s usually a third to a fifth of the cost of doing an in-lab study, and it’s typically covered by insurance,” he says.
Choosing the Right HST Device
When considering an HST, practitioners should know that not all sleep diagnostic home tests are created equal.
“The push for simpler sleep tests has sometimes risked sacrificing accuracy for simplicity. We have seen that most clinicians want to hit the sweet spot of simplicity and accuracy with their diagnostic tools,” claims Helgason.
The Nox T3 comes with analysis and reporting sleep software, Noxturnal, which help give a comprehensive picture of the patient. Recent research shows that Noxturnal’s automatic scoring system can accurately analyze AHI events comparable to manual scoring of Nox T3 recordings. Another study published in the journal Sleep and Breathing found that the Nox T3 portable monitor could detect even mild OSA.
“Nox T3 gives a comprehensive picture of the patient due to the amount of channels and inputs the device will gather. This is possible because Nox Medical is always striving to reduce the complexity of sleep studies, but, most importantly, without jeopardizing the integrity and amount of data gathered,” says Helgason.
Home sleep studies like the Nox T3 device, backed by clinical research to effectively diagnose OSA, allow sleep physicians to diagnose patients faster, even when they are hundreds of miles away. “The main benefit of home sleep studies over lab sleep studies is the vast difference in accessibility of the studies between technologies used and the healthcare resources required to perform the studies,” says Helgason.
As public awareness of sleep disorders among Americans continues to rise it appears like more people are seeking treatment for their sleep disorders than ever before. Currently, 50 to 70 million U.S. adults have a sleep disorder, which is often associated with obstructive sleep apnea (OSA), according to the American Sleep Association.
The Nox T3 Sleep Monitor
The sophisticated home sleep monitoring device, the Nox T3 by Nox Medical, can detect subtle changes in breathing throughout the night. The downloadable data gives clinicians a comprehensive picture of abdomen and thorax respiratory effort and derived flow, nasal cannula flow, body position and activity, as well as blood oxygen levels, and pulse. With these details, practitioners have the ability to refine their diagnosis.
Photo by Bryce Evans on Unsplash
Topic: Industry News